Basic Concept: CCHMC is a “special delivery service” and does not perform non-OB surgeries on pregnant patients.
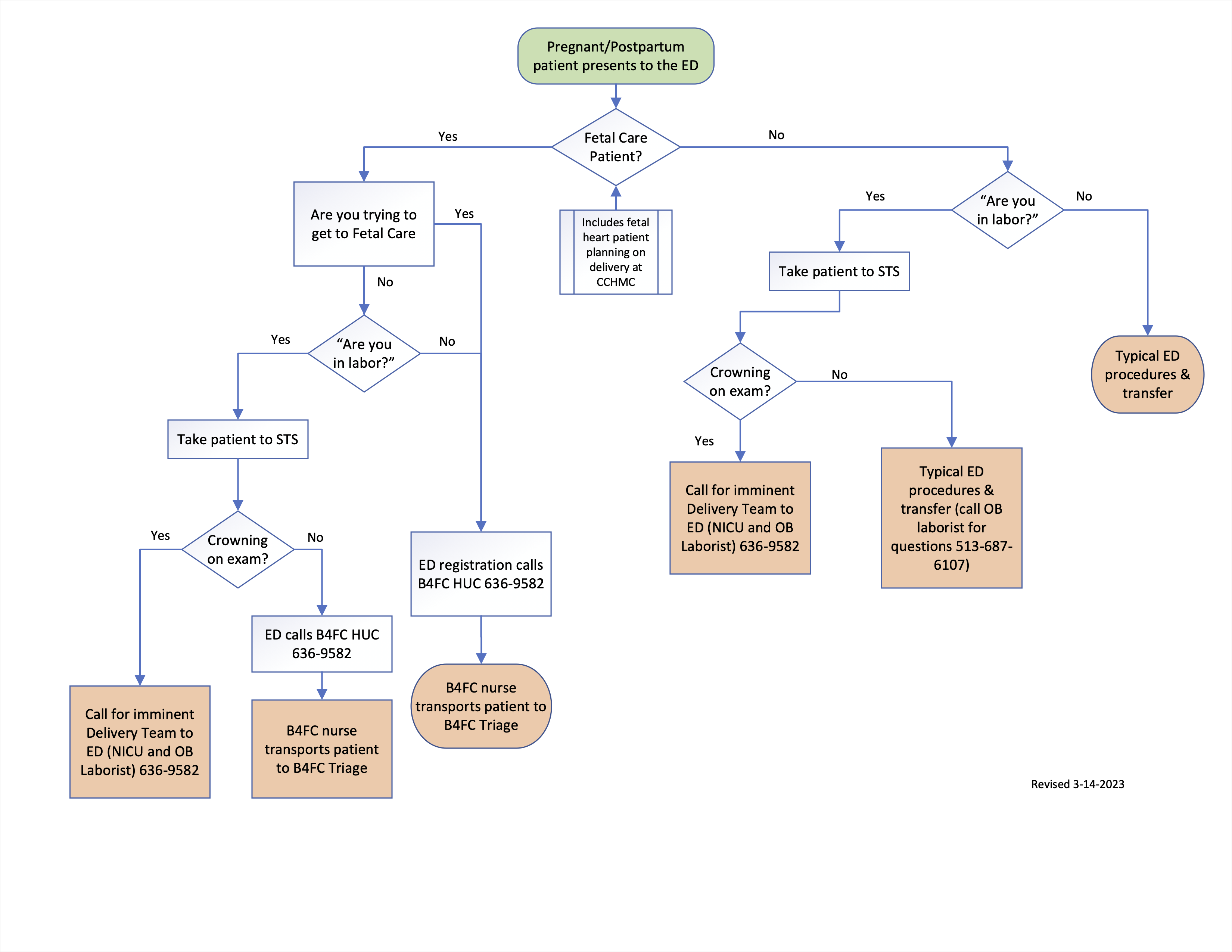
General recommended protocol for pregnant or postpartum patients presenting to the ED:
1) Patient is followed by the Cincinnati Fetal Center ➞ directed immediately to the B4 Fetal Delivery Unit
2) Patient is NOT followed by the Cincinnati Fetal Center ➞ ED evaluates and transfers patient to appropriate facility. Contact CCHMC OB Laborist (B4 Fetal Care) or Imminent Delivery Team (OB & NICU included) only as needed.
These recommendations were determined by staff from the ED, MFM, Gyn, and Legal Services at both CCHMC and TriHealth.
FOR IMMINENT DELIVERY CALL 636-9582; that is the B4 Fetal Care Unit Coordinator – ask for “Delivery Team to the ED” (activates OB & NICU)
FOR OB questions call 513-687-6107; that is the OB Laborist in B4 Fetal Care (available 24/7)
NICU Only Resuscitation Team Activation Process
- Criteria for Activation
- Any newborn <12 hours old requiring intubation
- Any newborn <12 hours old in cardiac arrest (NRP indicated)
- Any newborn followed by the Fetal Care Unit regardless if pre-term or term (delivered at home, en route, or in the ED)
- How to Activate
- Call 69582 (Fetal Care Unit HUC Desk)
- Request the NICU ONLY Resuscitation Team to the ED (AKA RED ALERT)
- Provide specific criteria met for activation
- Any newborn <12 hours old requiring intubation
- Any newborn <12 hours old in cardiac arrest (NRP indicated)
- Fetal Care Newborns
- NICU Arrival
- Team includes NICU Attending, fellow, APP, RT, RN’s 2-4, and PCA
- Neonatal Resuscitation Resources in the STS
- Generic Code Medication Sheets (in PINK Binder in bottom drawer of med counter)
- Neonate drug kit for <12 hour old patients (search NEO or KIT)
- Scan barcode twice (1st when it asks to scan, second when it asks for serial code)
- Co-sign sheet in kit with NICU RN prior to returning kit to pharmacy
- 8th ed NRP algorithm in the MRC binder
- Delivery Cart
- ED team will transition care to NICU Team upon their arrival
- ED Team Leader and Two ED RN’s will remain with the patient to document in EPIC and assist with removing medications from Pyxis, getting equipment, general way finding in the STS
** For all other infants not meeting the above listed criteria, call the NICU Fellow as needed/indicated for consults, planned admissions, etc,.
Precipitous Deliveries: Medications for All Newborns
Erythromycin Eye Ointment
- Availability:
- Burnet ED: STS3 Pyxis machines
- Liberty ED: North and South Pyxis machines
- Prophylaxis for neonatal gonococcal ophthalmia
- 0.5-1 cm ribbon of ointment should be instilled into each conjunctival sac immediately after birth
- Administration technique:
- Wipe each eyelid gently with sterile cotton; instill 0.5-1 cm ribbon of ointment in each lower conjunctival sac; massage eyelids gently to spread the ointment; after 1 minute, excess ointment can be wiped away with sterile cotton
Vitamin K (Phytonadione)
- Availability:
- Burnet ED: STS 3
- Liberty ED: obtain from pharmacy
- Prevention and treatment of hemorrhagic disease of the newborn
- Prophylaxis Dose: 1 mg IM within one hour of birth
Hepatitis B Vaccine (Engerix-B®)
- Not available in the Emergency Department; obtain from pharmacy
- Dose: 10 mcg/0.5 mL IM x 1 dose
- If newborn is healthy and transferred to UC, may defer dose until patient is transferred
- Neonates born to HBsAg-negative mothers:
- Birthweight <2 kg: Administer initial dose at 30 days of chronological age or at hospital discharge (whichever is first).
- Birthweight ≥2 kg: First dose should be administered within 24 hours of birth.
- Neonates (regardless of weight) born to HBsAg-positive mothers:
- First dose: 0.5 mL within first 12 hours of life, even if premature and regardless of birth weight; hepatitis B immune globulin (HBIG) should also be administered at the same time at a different anatomical site.
- Neonates born to mothers whose HBsAg status is unknown at birth: First dose given within 12 hours of birth even if premature regardless of birth weight
